The diagnostic testing that has traditionally been used to evaluate brain injury has consisted of imaging that looks at the brain structure like CT, MRI, PET, or SPECT scans. While these can be quite useful, they are often negative in patients with traumatic brain injury as they don’t tell us much about brain function.
The diagnostic testing we use in our offices to help evaluate traumatic brain injury is designed to measure problems with brain function, rather than structure. By evaluating eye movements, balance, brain waves, memory, reaction time, sleep problems, and other parameters we are able to better understand the ideal treatment options for brain injury.
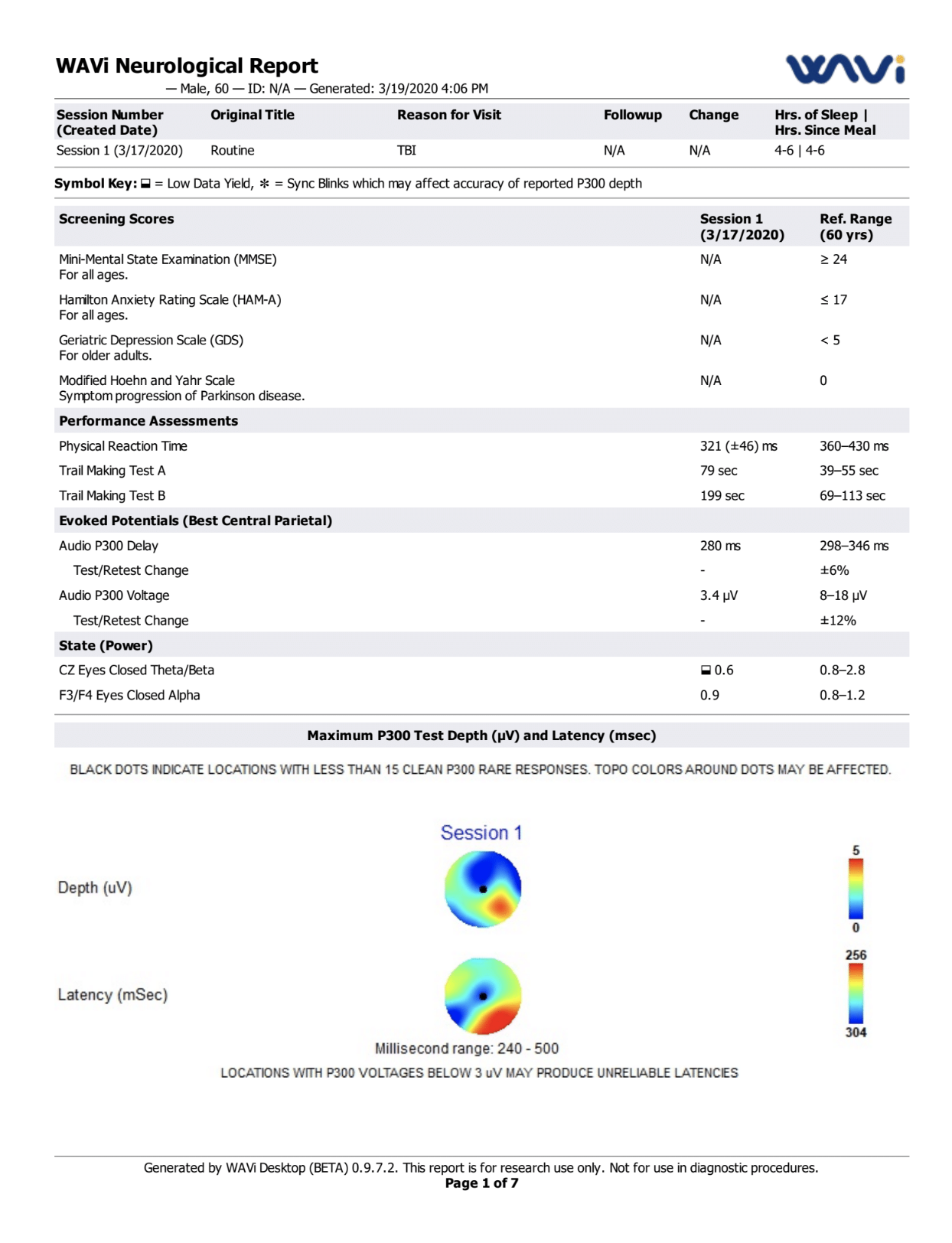
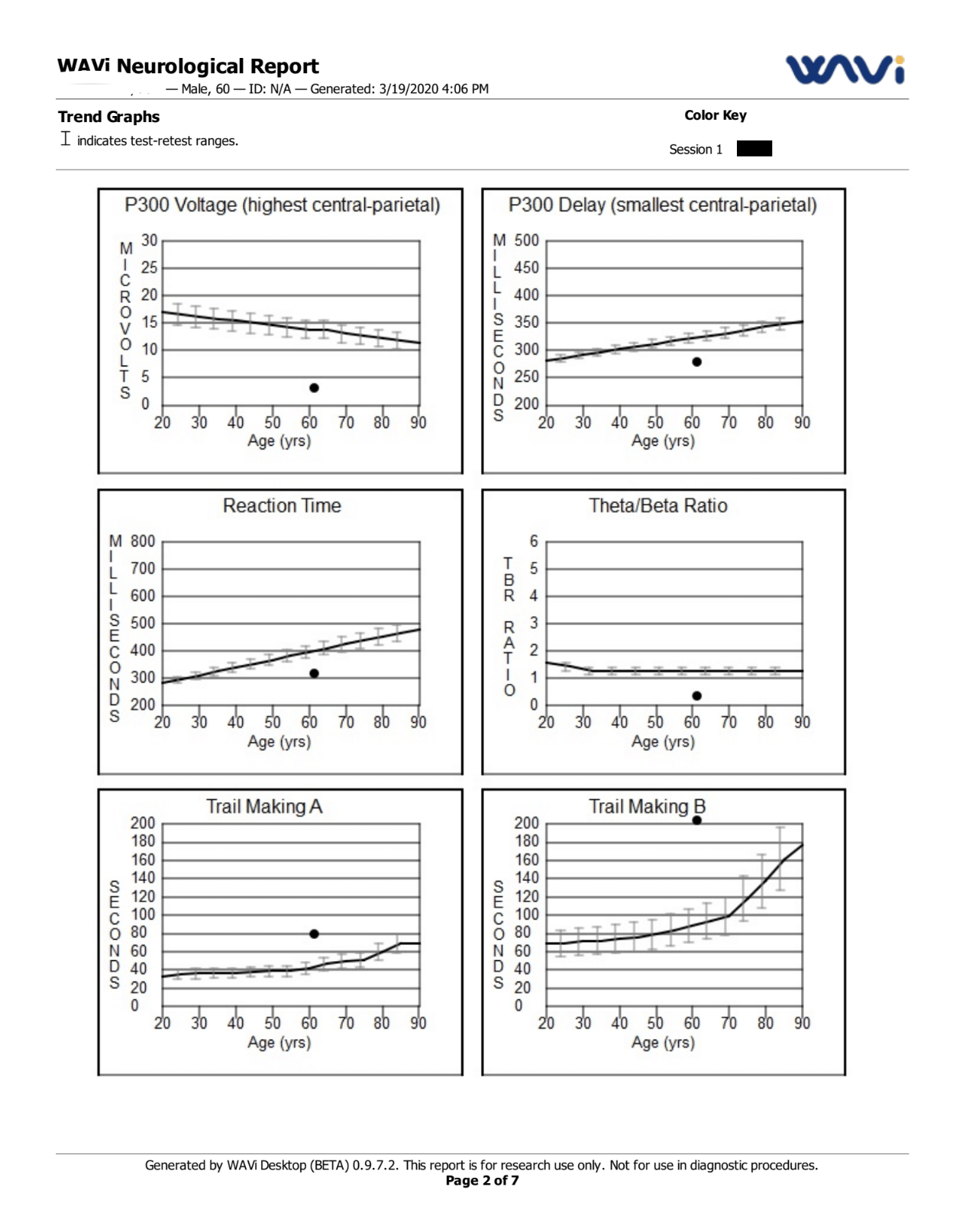
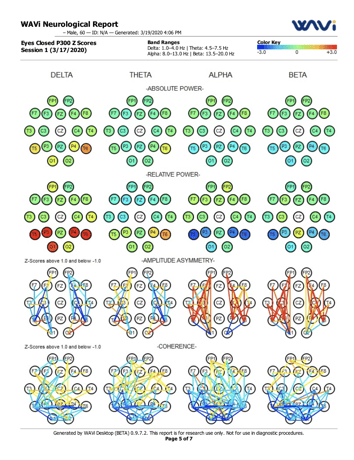
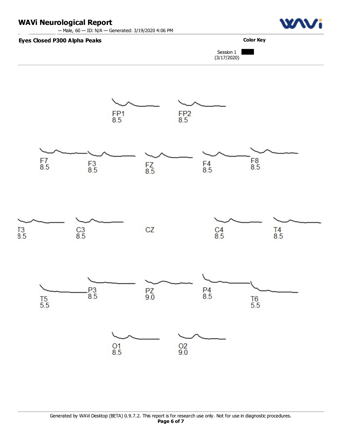
EEG is one of the most commonly used tools in the neurology world for evaluating the electrical activity in the brain. While EEG testing alone does not prove or disprove the presence of TBI, it can provide valuable insight, particularly when used in conjunction with a comprehensive battery of diagnostic tests.
The EEG device we use also can also evaluate how the brain responds to visual and auditory stimuli (visual evoked potentials and auditory evoked potentials) to better assess any abnormalities in function.





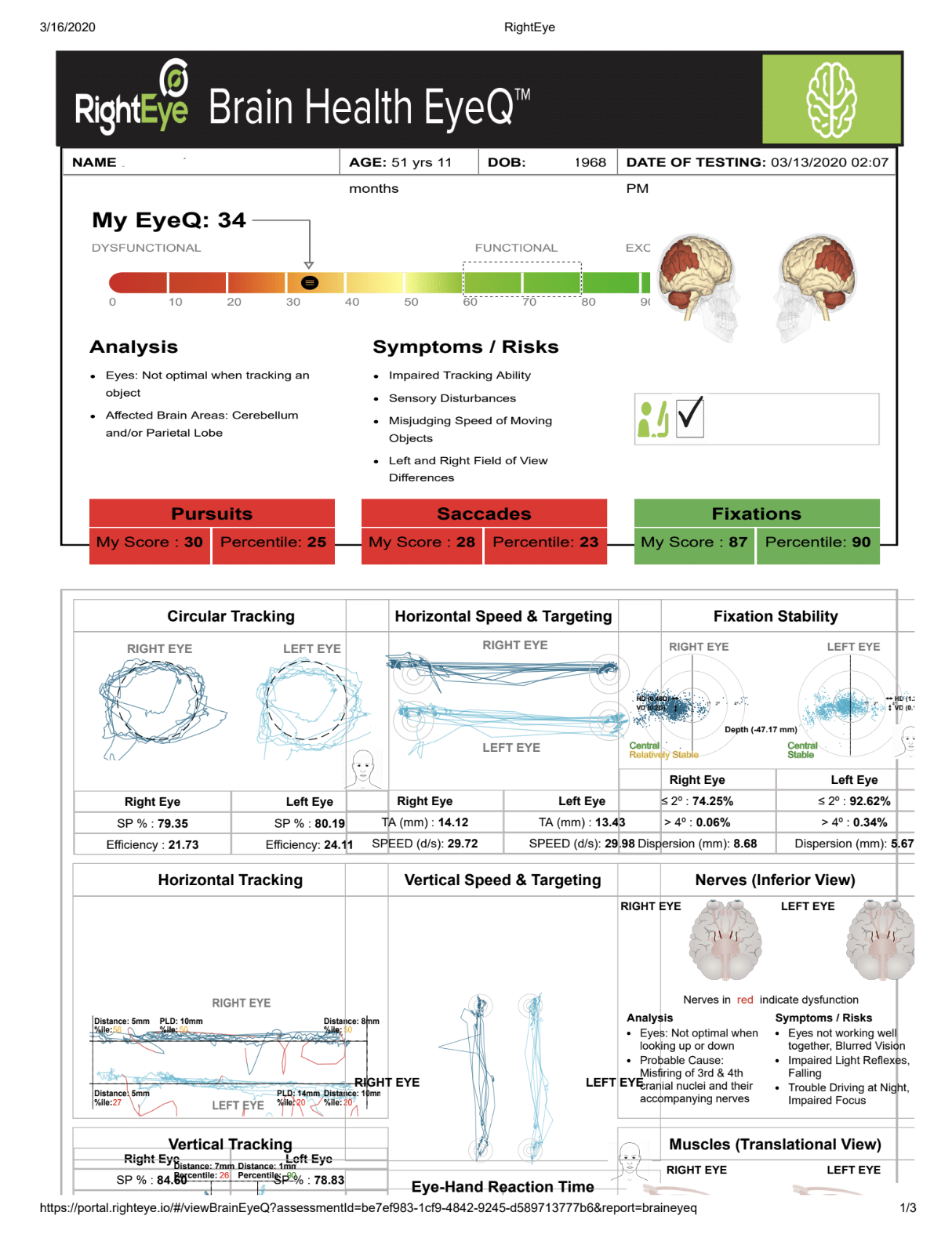
While VNG testing is observing the movements of the eyes, oculomotor tracking technology allows us to see what the eyes are following. This is of great importance because one of the most common symptoms of TBI is disrupted communication between the eyes and the brain.
When this happens, the eyes do not follow objects properly as we move our heads or as objects are moving in the visual field. Oculomotor tracking can provide very visually compelling information as to just how dysfunctional eye movements might be.
In the image on the left below you can see what normal eye-tracking should look like when the subject is instructed to follow a circular path. The image on the right stands in sharp contrast, demonstrating what can happen after traumatic brain injury.
The device we utilize is called the Right Eye, and in addition to serving as a valuable diagnostic tool, it also helps guide rehab exercises for the eye muscles. This is called sensory integration therapy, or oculomotor rehabilitation, and it can be of tremendous benefit in helping to restore normal function to the eye movements and aid healing from a concussion.



When the brain is injured, the sense of smell, known as olfactory function, is often altered. Many patients with TBI report alterations in their ability to smell or taste normally due to damage to the specific areas of the brain that control these functions. Our in-office olfactory testing allows us to assess any changes in these senses to better understand what areas of the brain have been affected.
Decreased balance and loss of coordination are some of the more commonly reported symptoms following traumatic brain injury. Studies show that between 30-65% of patients will report balance problems with TBI.
Injury to the brain can affect communication with the inner ear as well as the eyes, creating a sensory mismatch that can lead to balance dysfunction, dizziness, or vertigo.
In some patients, this becomes severe enough to become a danger to the patient as their fall risk increases.
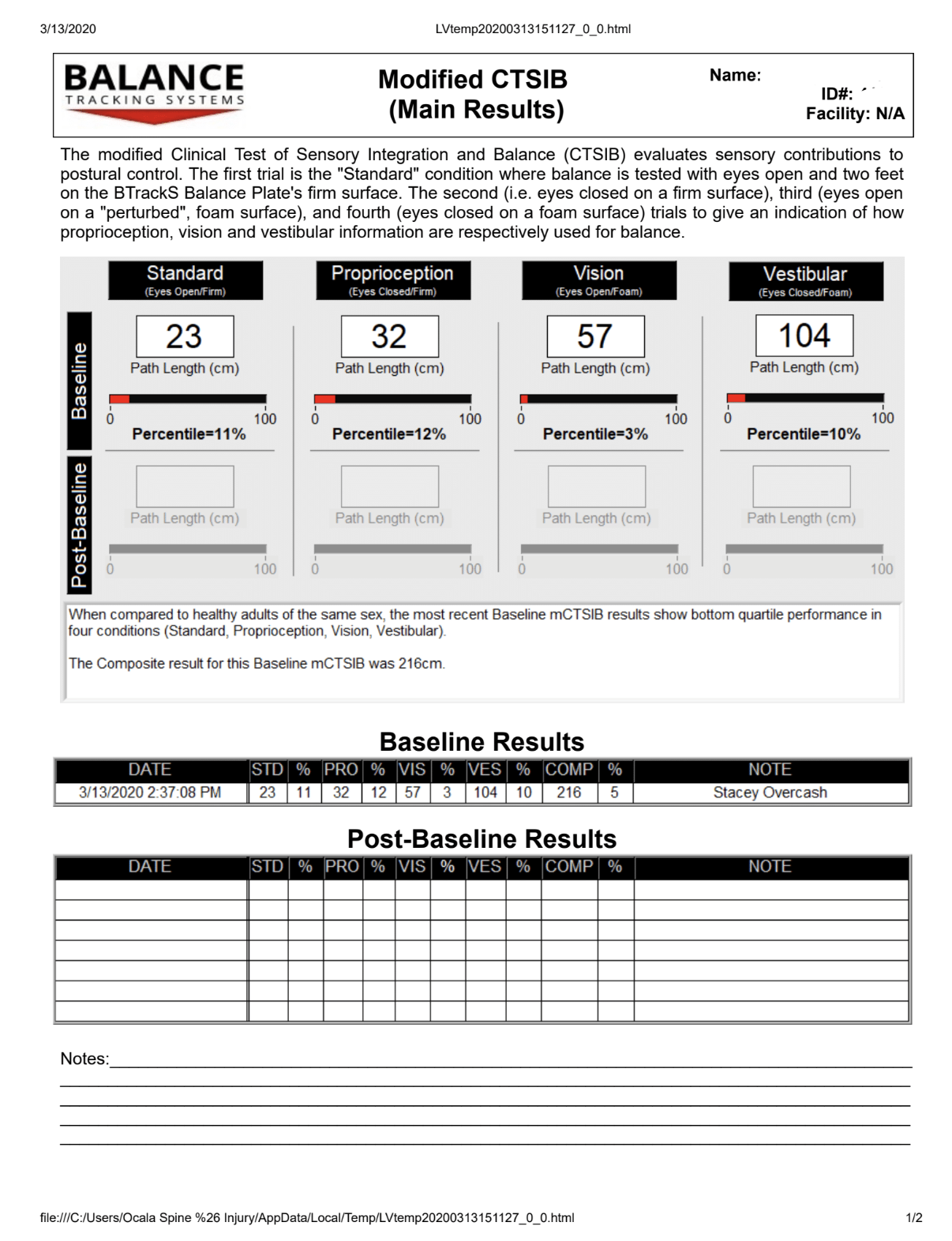
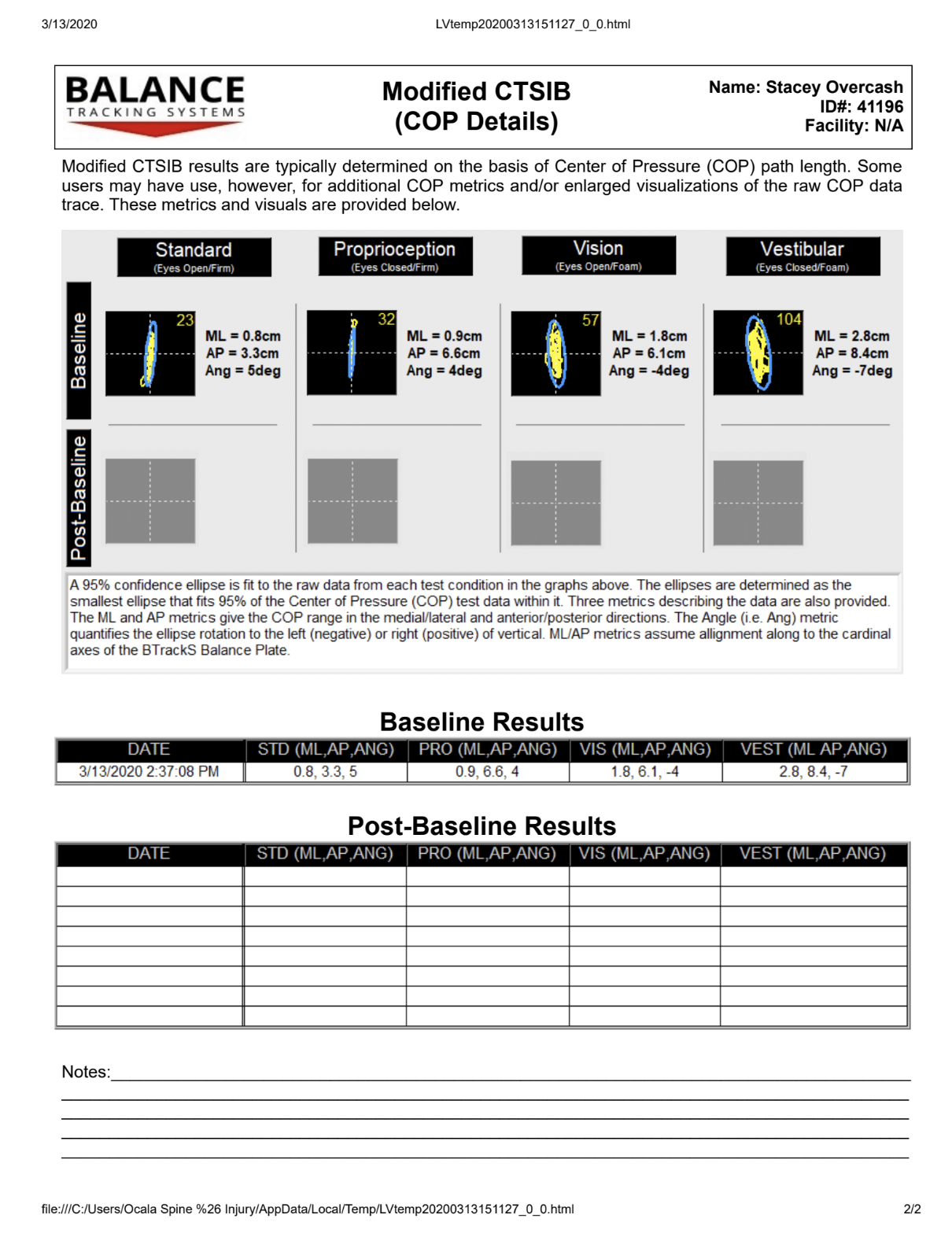
We utilize a specialized form of balance testing called computerized dynamic posturography that measures the amount of sway and loss of equilibrium experienced by the injured patient.
This data is not only helpful in providing objective evidence of problems related to TBI but can help guide the appropriate rehabilitation options for the patient to experience functional improvement.



Sleep disorders like insomnia are one of the more common symptoms that patients with traumatic brain injury will report. Proper sleep is critical to brain health and function, so when you are not getting quality restful sleep the effects can be devastating. We utilize polysomnography, also known as a home sleep study, to better evaluate the duration and quality of your sleep. This involves a non-intrusive testing device that is sent home with you so that you can be conveniently tested in your own home with minimal discomfort.
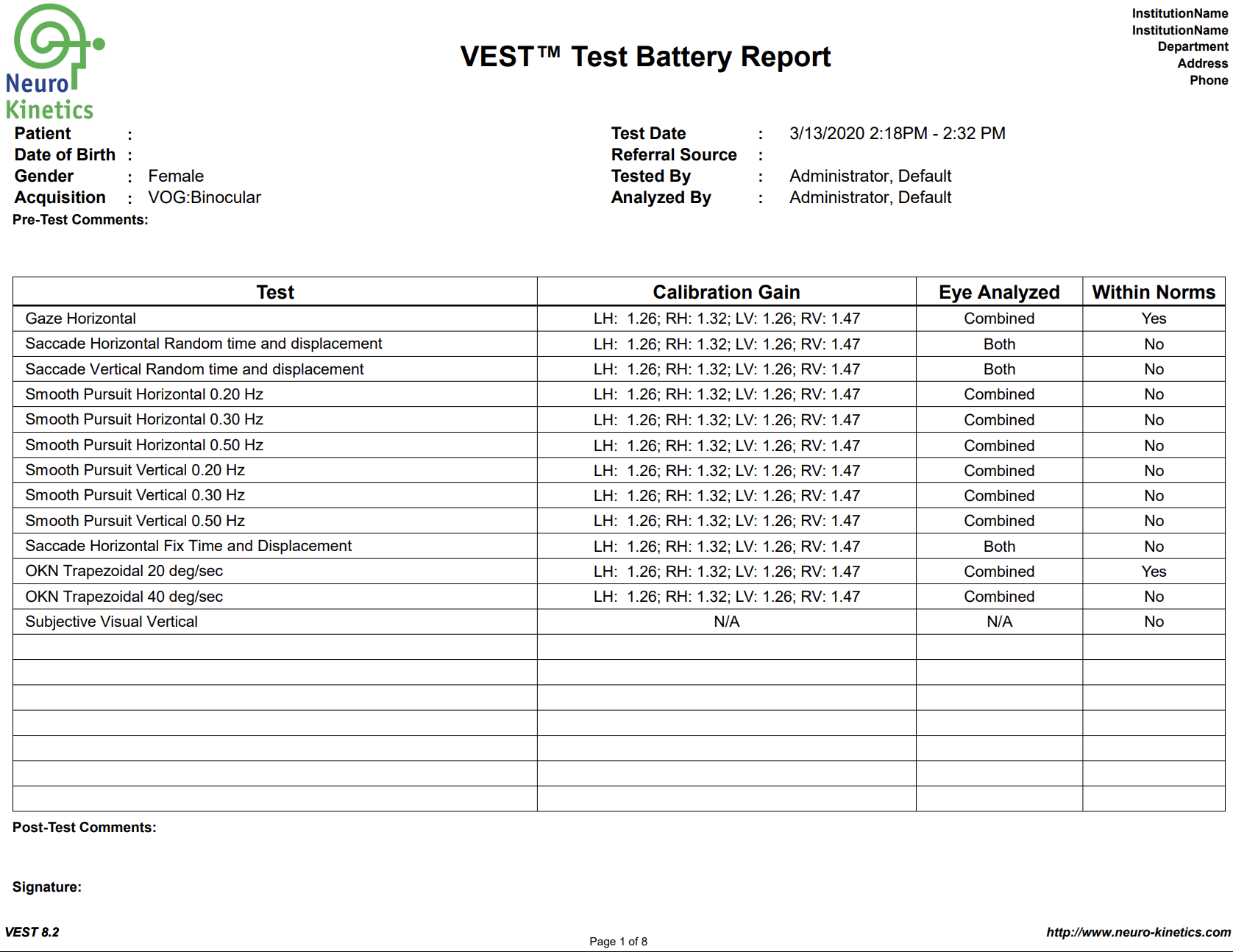
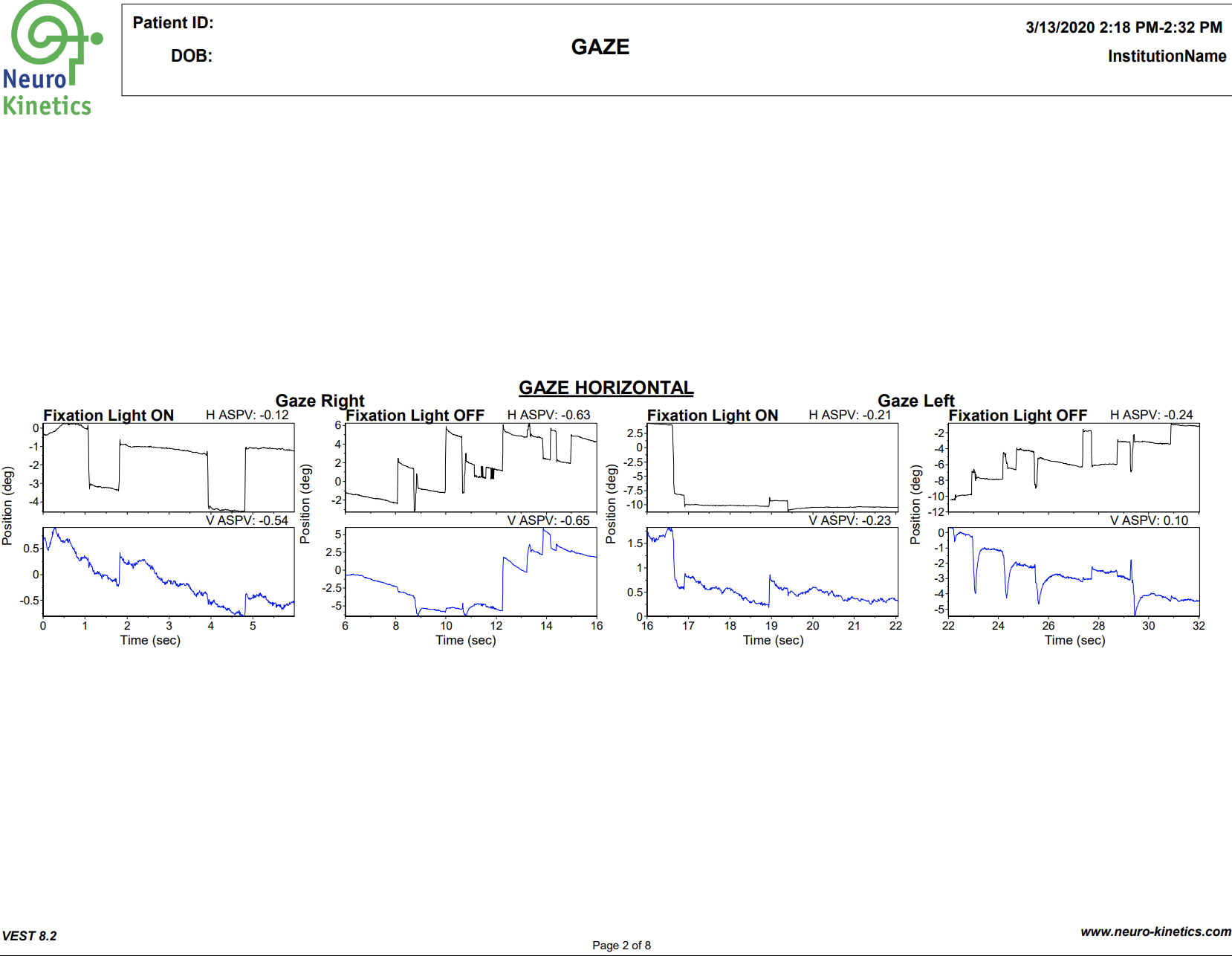
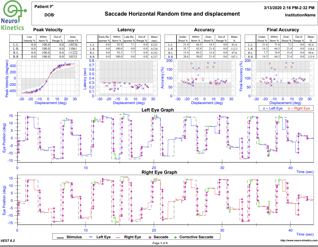
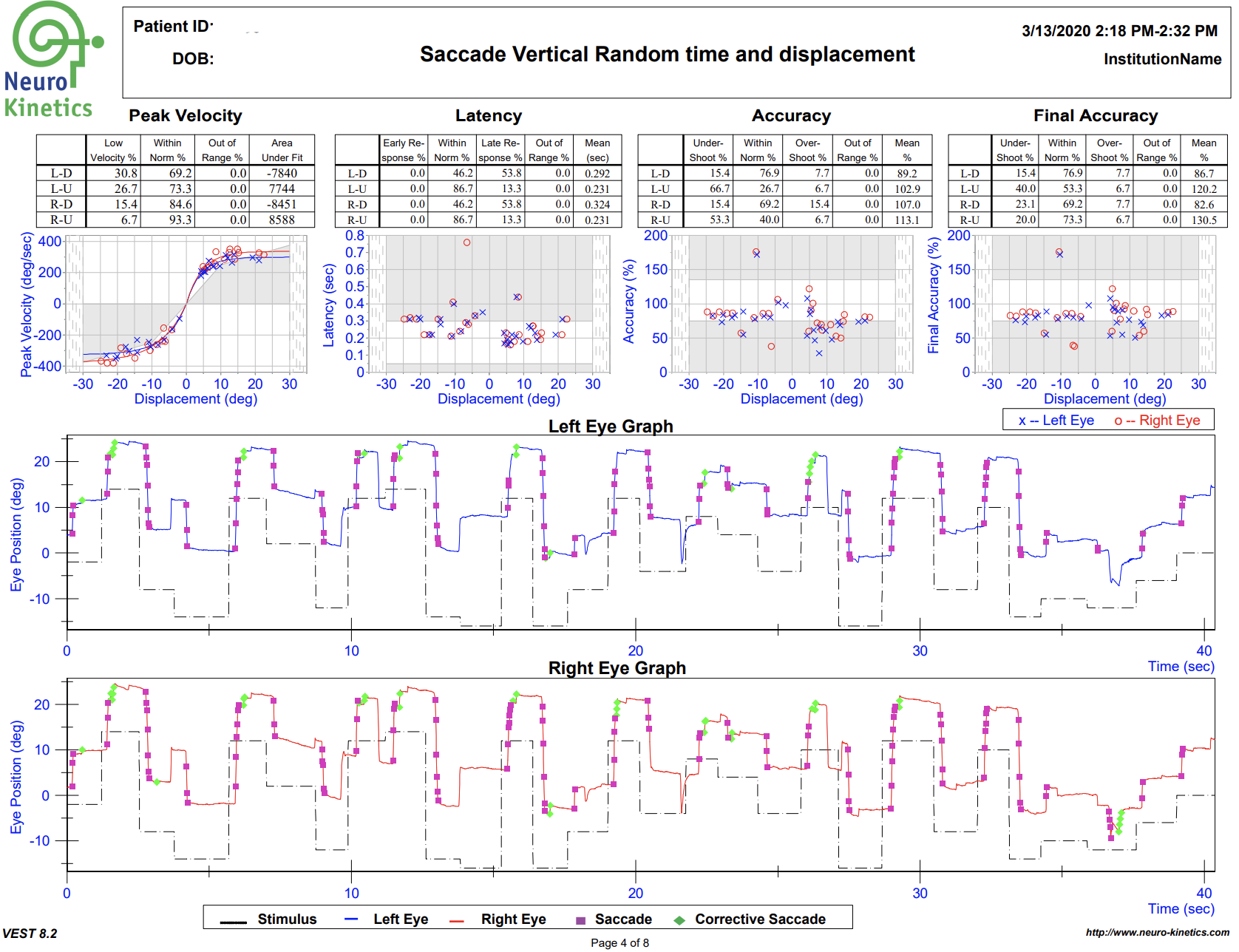
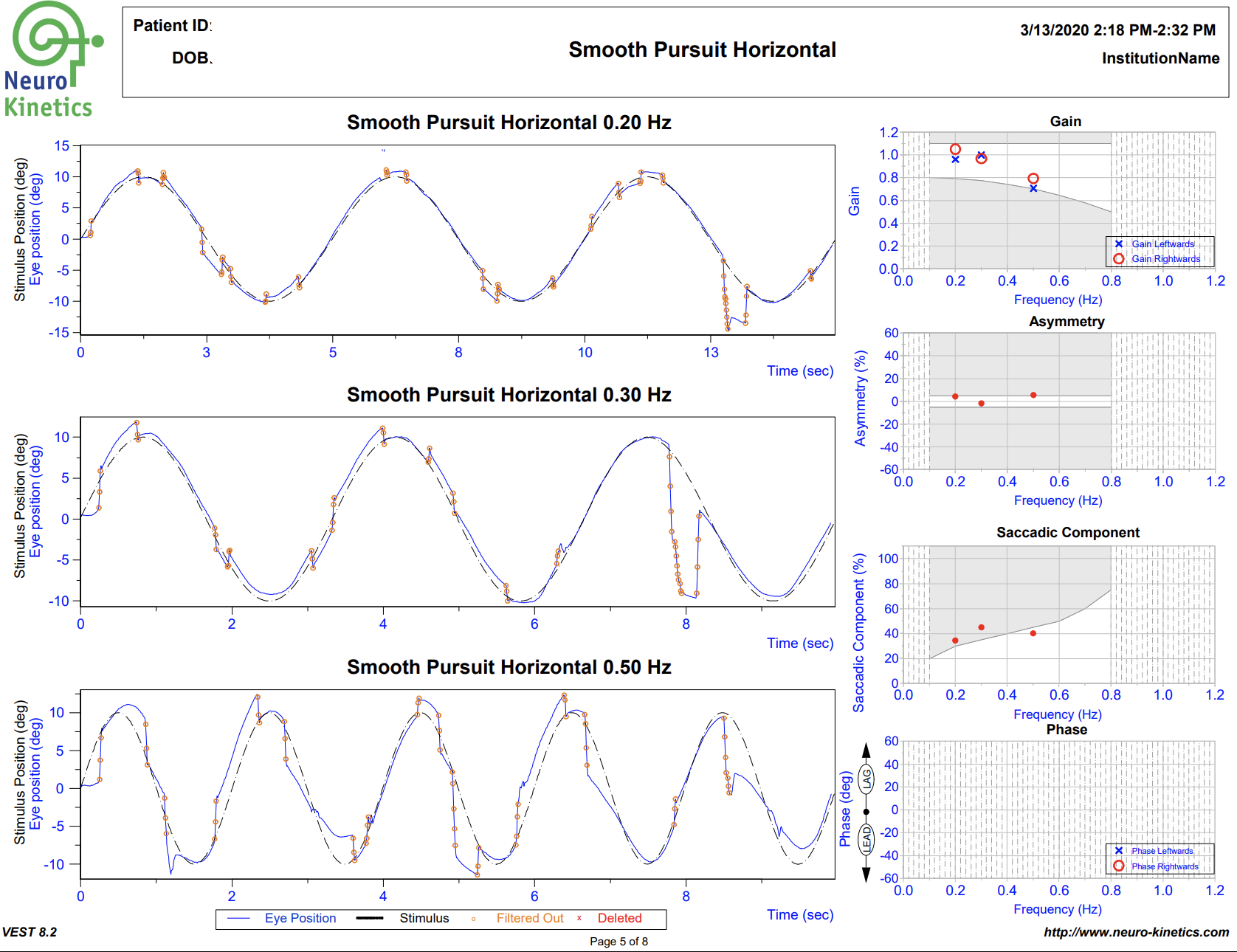
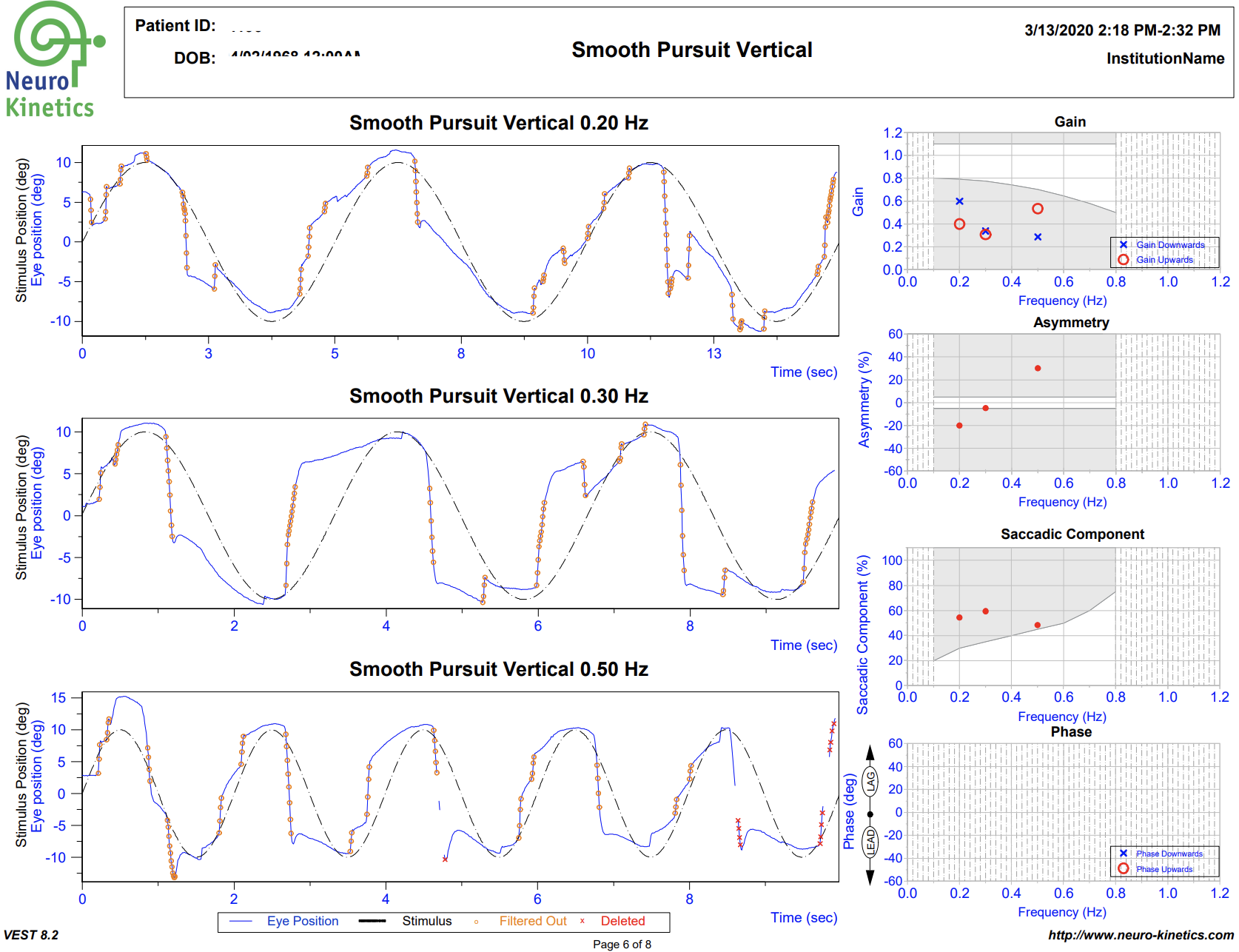
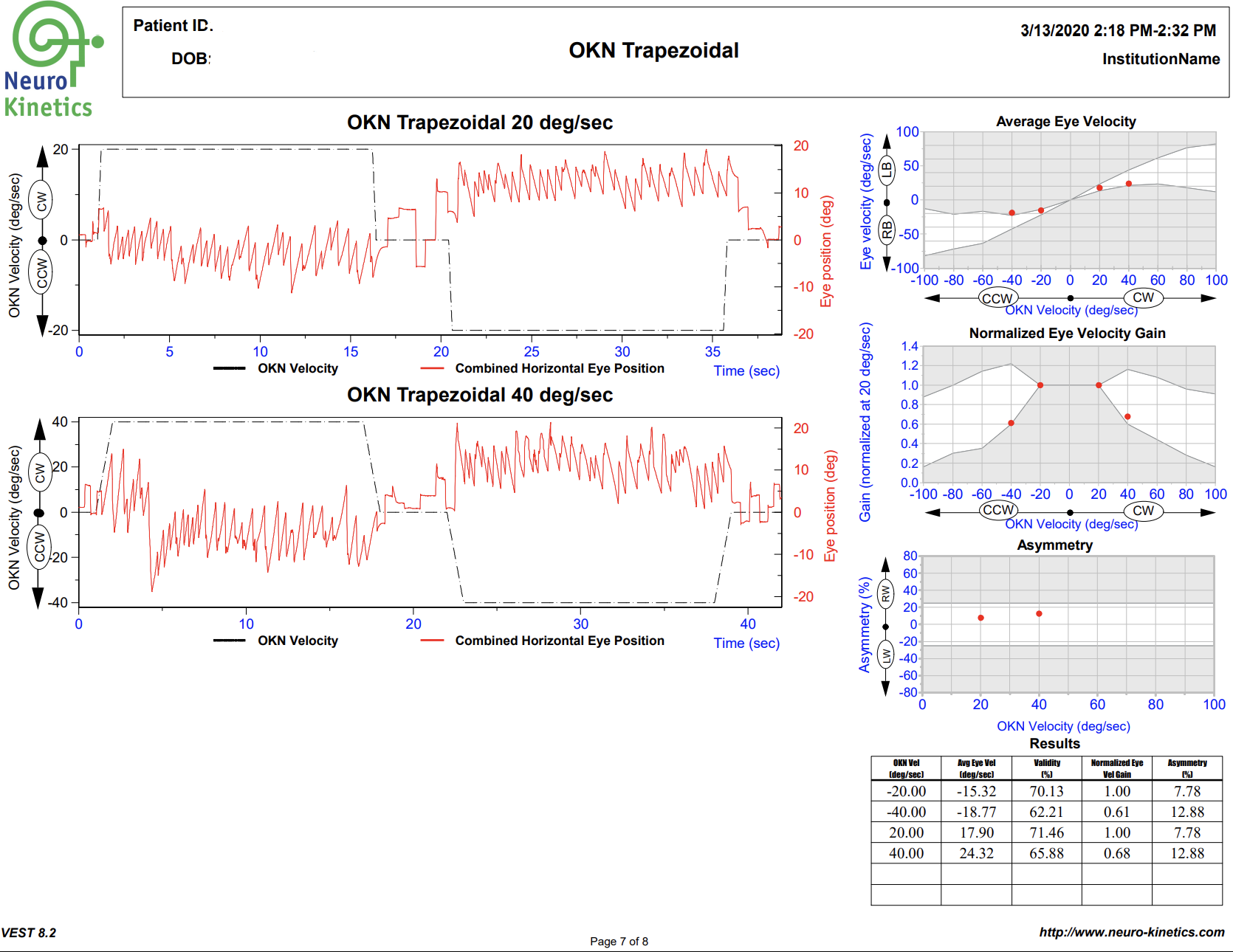
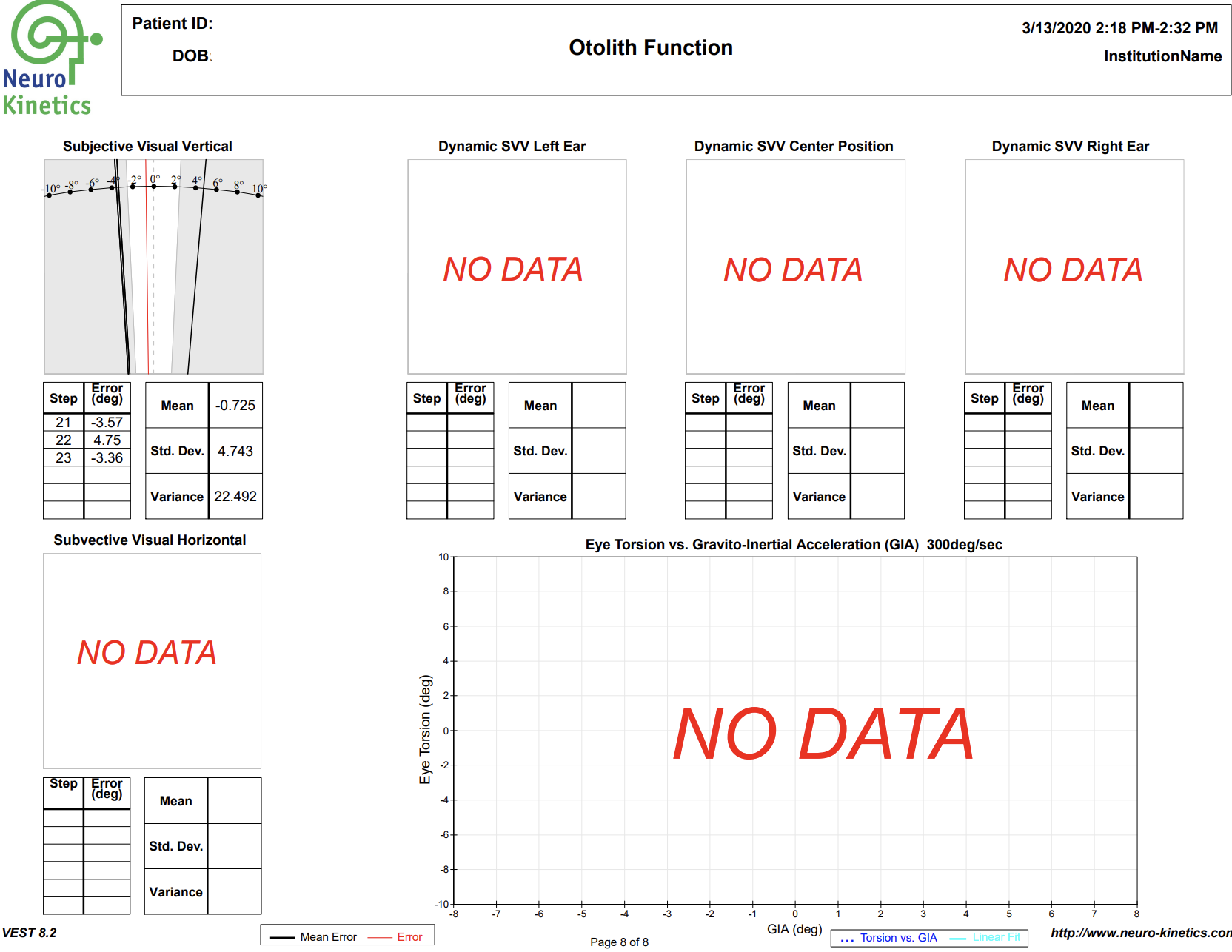
VNG testing uses small infrared cameras housed in a headset seen above to record subtle eye movements that can be altered following TBI. In most doctor’s offices and hospitals, the assessment of eye movements are done with the classic “follow my finger” test and other exam procedures which often do not pick up on more subtle dysfunction.
The FDA cleared technology allows us to graph the eye movements and compare them to healthy subjects, giving compelling objective data of TBI.
This technology has been used for years in university research settings, highly specialized neuro-ophthalmology practices, and hospitals; but recent advances make this equipment practical for use in private practice.
A standard physical examination relies on the keen observation and interpretation of the doctor, while VNG testing allows us to gather much more concrete, objective data of any dysfunction that may be present.

The autonomic nervous system (ANS) controls unconscious activities like heart rate, blood pressure, and respiration. TBI often causes dysregulation of this part of the nervous system, particularly the sympathetic (also known as the “fight or flight”) portion.
Studies place the incidence of ANS dysfunction following brain injury at 8-33% of patients. Imbalances in the nervous system tend to drive up anxiety, blood pressure and have even been implicated in long term increases in cardiovascular-related death.
We measure ANS function by evaluating heart rate variability (HRV) with a device that assesses pulse waves as well as respiration. HRV is a well-established method of assessing how the body is adapting to stress, one of the primary responsibilities of the ANS.

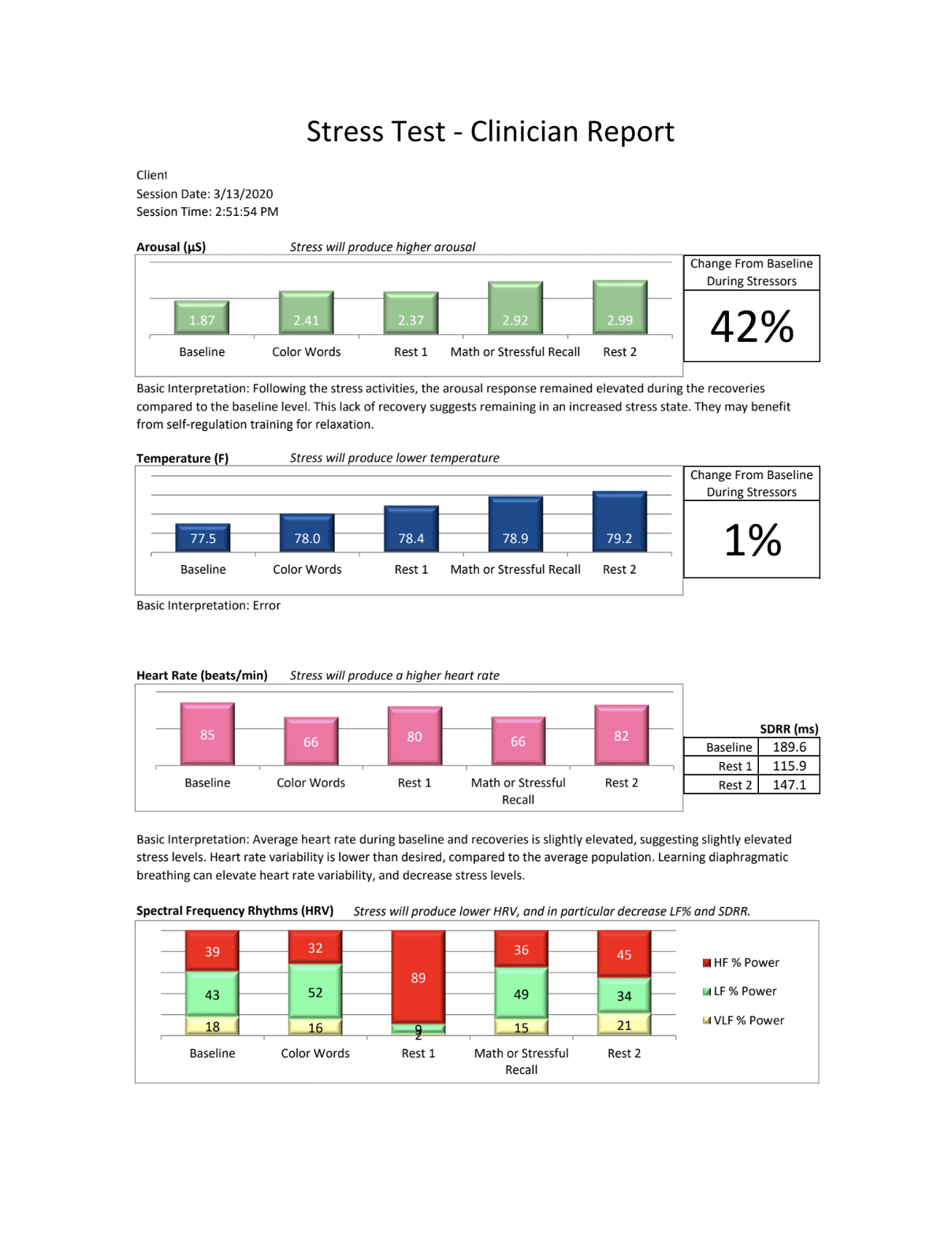

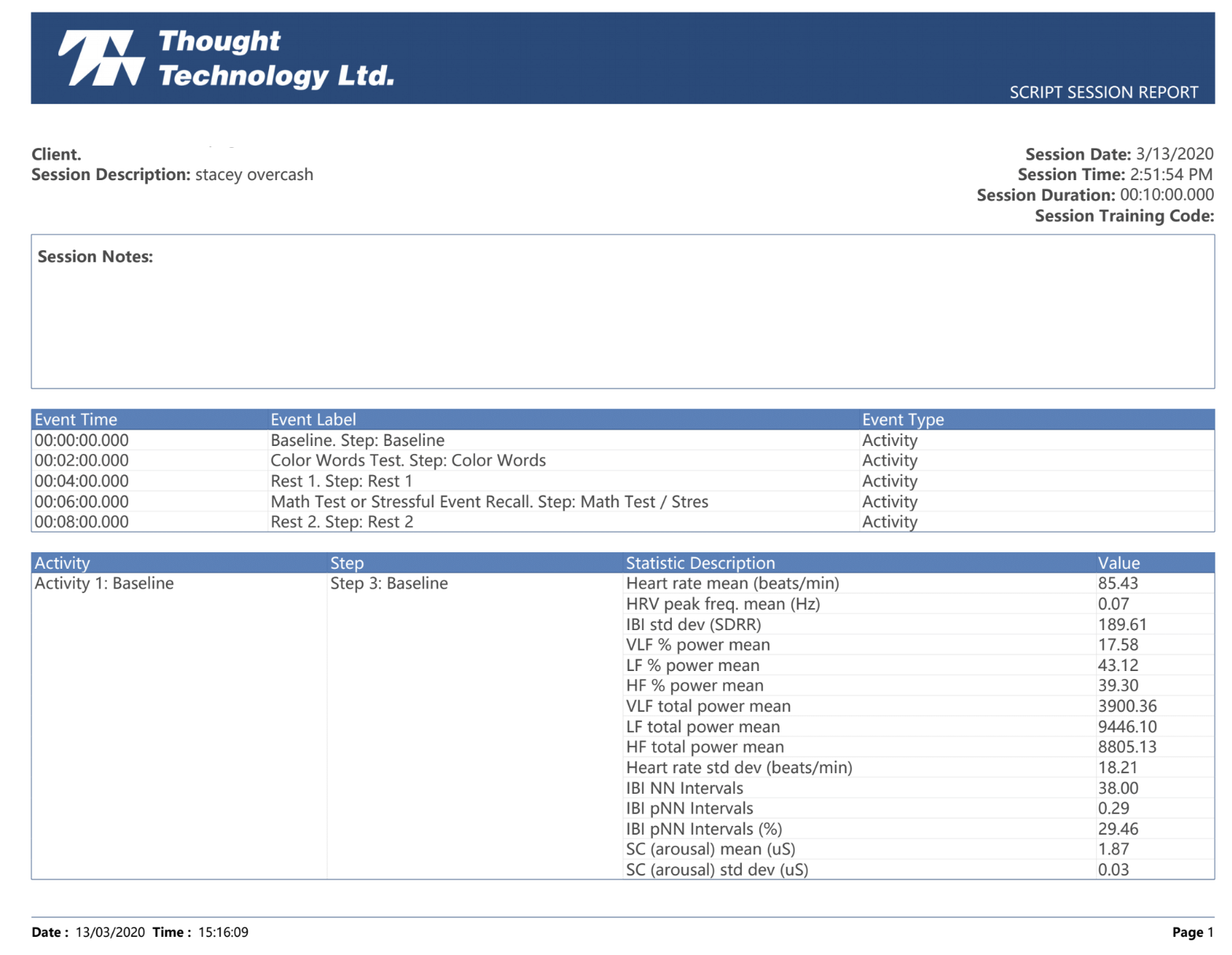
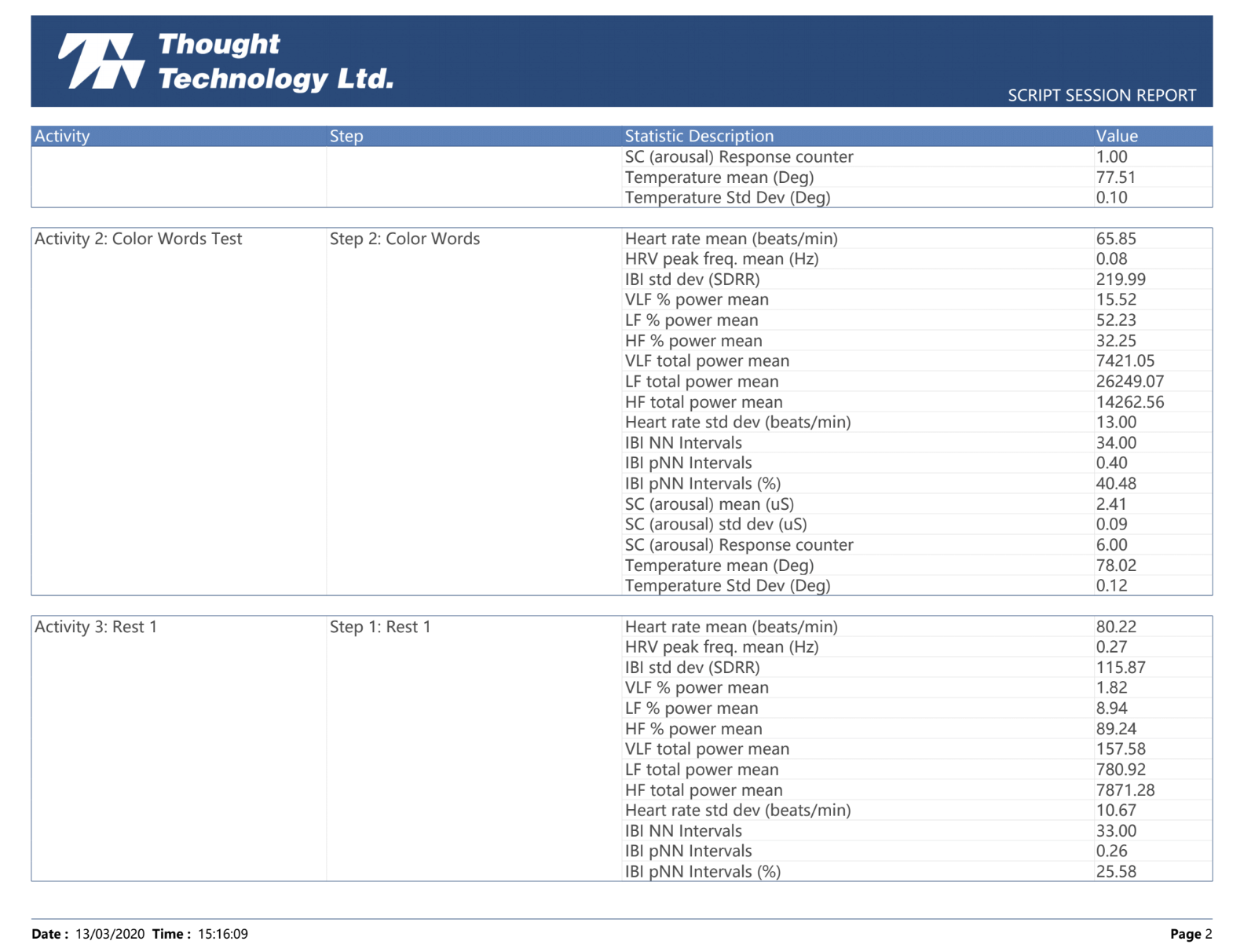
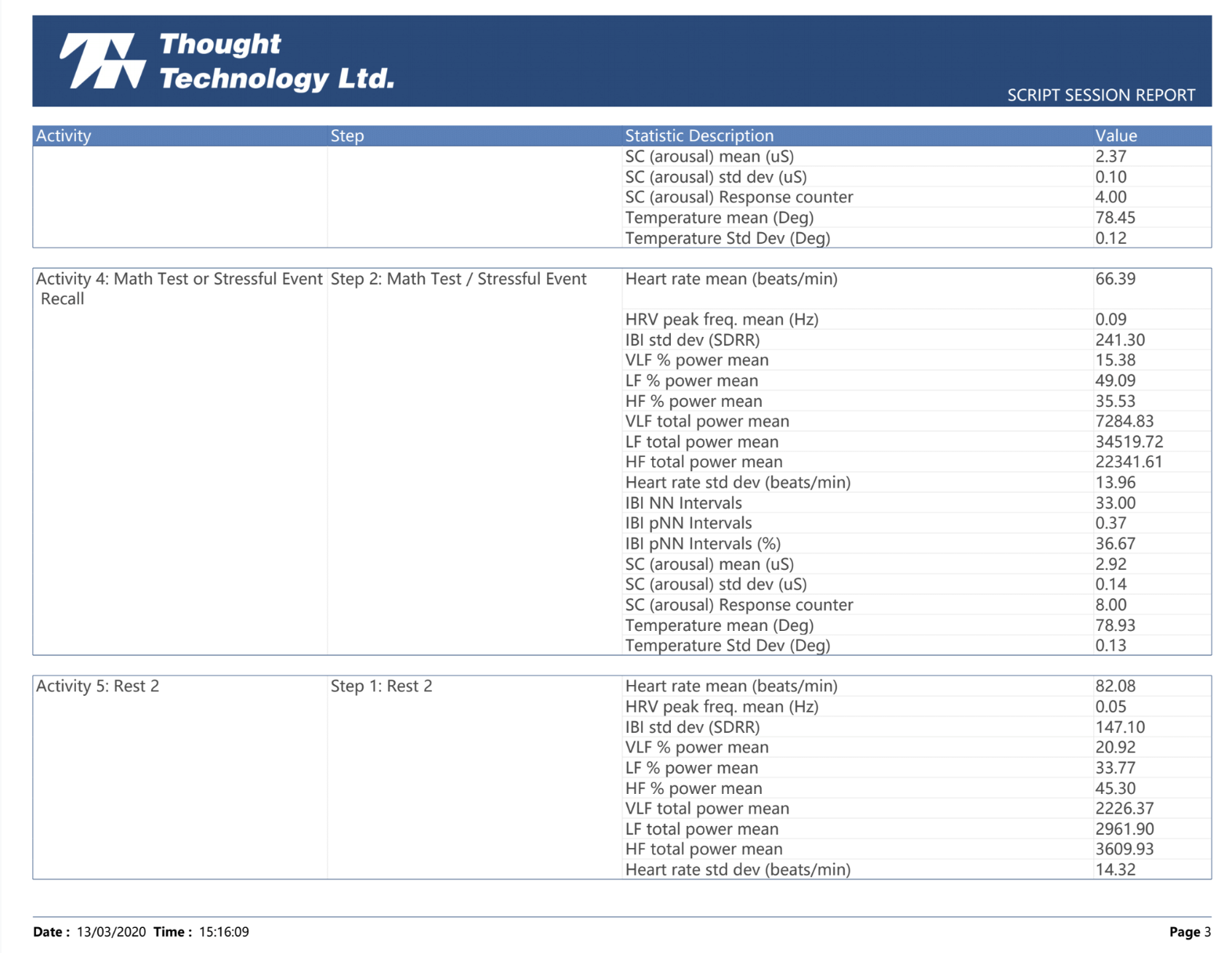
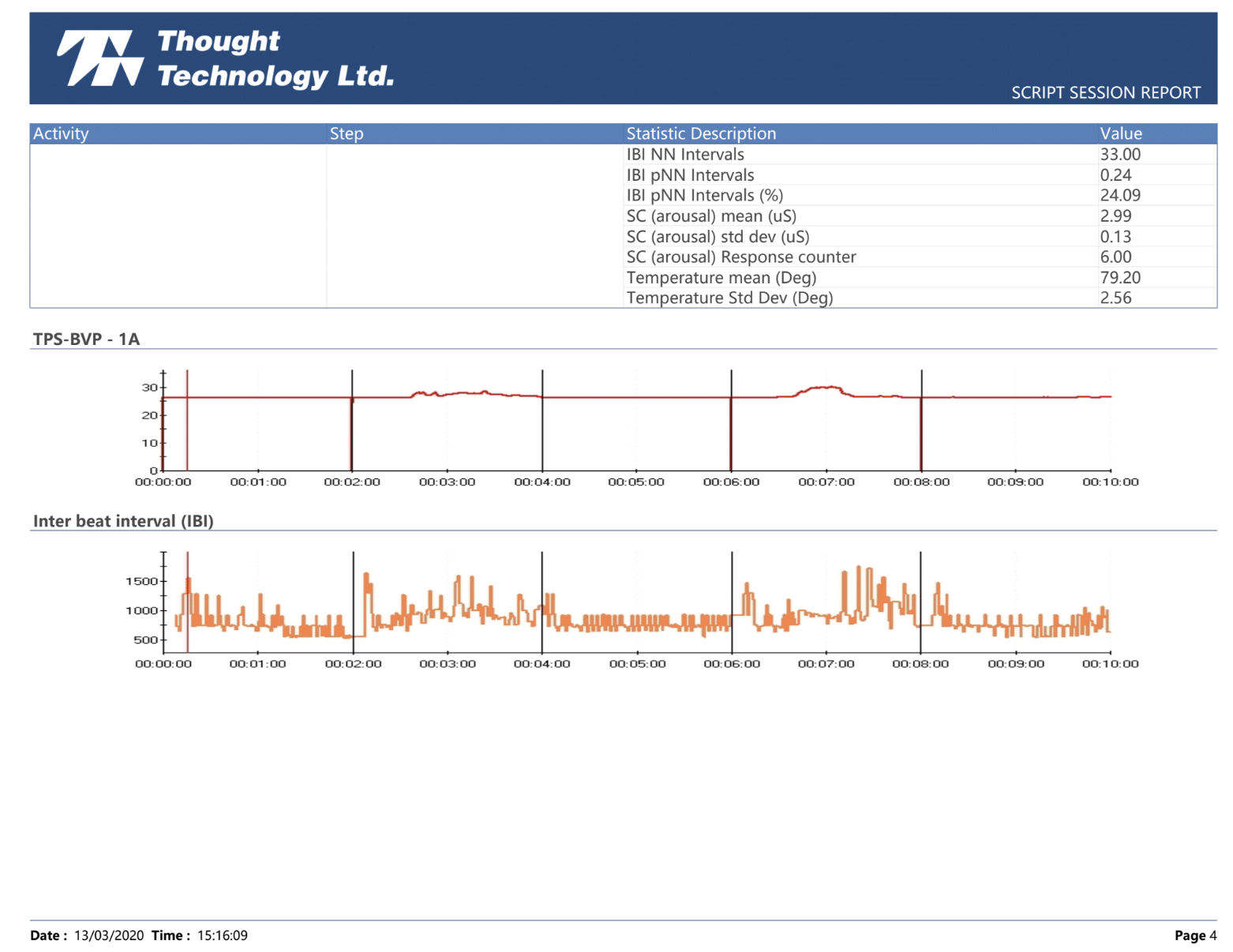
Many people are not familiar with some of the specific TBI testing that we perform, and the reports can seem rather technical in nature. This video is designed to give a brief overview of the tests, and show the context of some normal vs abnormal images. Our goal is that this short tutorial will make the clinical implications of the diagnostic studies easier to understand.